Nova Scotia Health and EY collaborate to digitally transform
Canadian healthcare provider Nova Scotia Health has been working closely with leading global consulting firm, EY, to use data and insights to better serve its clientele.
“We’ve been working collaboratively with Nova Scotia Health, supporting them through their ambitious digital transformation agenda,” says Steven Maynard, EY Canada Government & Public Sector Consulting Leader. “Having worked with others on similar journeys, both across Canada and around the world, we know how increasingly important data – and making insights consumable to clinicians – has become to improving overall outcomes in healthcare.”
In addition to its digital transformation, the organisation has restructured to evolve over the years. Prior to 2015, it was composed of nine separate district health authorities.
“Nova Scotia Health is now the single provincial health authority covering the entire population of the province,” says Matthew Murphy, Senior Director, Strategy and Performance and Chief Data Officer at Nova Scotia Health. “We provide care across the entire spectrum of care, from public and primary health care to acute care, as well as long-term and continuing care.”
Unlike other for-profit public healthcare systems around the world, Canadian healthcare operates under a single-payer, publicly-funded system, with each province administering healthcare in alignment with the Canadian Health Act, and Nova Scotia Health is no different.
“We have the benefit of administering the entire spectrum and that really comes into play when we start looking at how we plan services and deliver care to meet the needs of the population,” says Murphy. “We use analytics to support that delivery of care because it gives us access to information across the entire patient journey.”
Ambitious healthcare goals
Nova Scotia Health has a broad purview when it comes to healthcare operations in the region. Due to this positioning, the organisation is able to map a patient's experience from beginning to end to best understand the resources and interventions needed along the way.
“Understanding what has happened in the past and using that to plan for the future helps us identify where new innovative technologies or approaches might be able to be leveraged in something like virtual care,” continues Murphy.
As part of the journey-mapping process, Nova Scotia Health recognised that, across the province, not everybody had equal or equitable access to services.
“One of the core focuses in the last couple of years has been to team up with different organisations or consultancies, like EY, to leverage their expertise in priority areas that Nova Scotia Health is driving toward but lacks the bench strength to fully deliver,” says Murphy.
“We work really closely with our analytics team and have scientists and some of our own people focused on evaluation, but we do everything in partnership, which is, I think, quite different from other organisations,” says Dr. Gail Tomblin Murphy, Vice President of Research, Innovation and Discovery, and Chief Nurse Executive at Nova Scotia Health.
Backed by over 300,000 people around the globe and with a purpose to build a better working world, EY Canada’s Government and Public Sector (GPS) and Health practices focus on helping organisations like Nova Scotia Health create new ways of working to achieve better outcomes for its citizens and better experiences for its employees.
“Our work with Nova Scotia Health has been in support of its vision to improve and deliver personalised healthcare services to the residents of Nova Scotia,” says Maynard. “We brought deep expertise and an understanding of the business of healthcare to help identify the big questions and advise on solutions that break through technical issues to deliver quality and value for patients, clinicians, government and the taxpayer.”
Evolving the digital landscape
The digital transformation of Nova Scotia Health was catapulted forward by the pandemic, which identified areas of vulnerability across the province’s healthcare system.
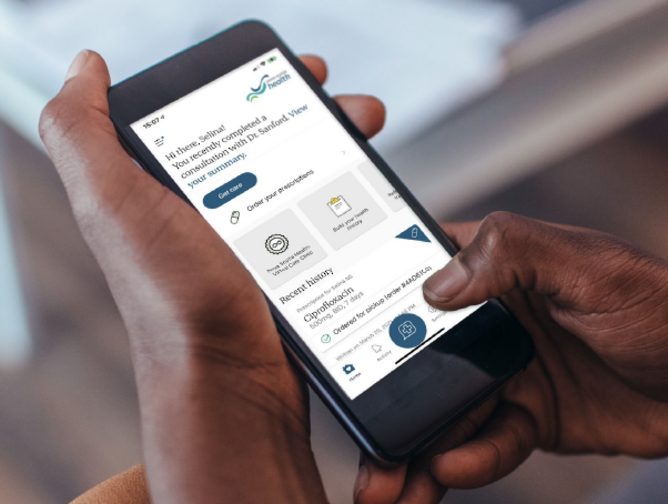
“A year ago, we saw an increase in the number of people in Nova Scotia who did not have a primary care provider,” says Tomblin Murphy. “We were asked to come up with an innovative solution to link each unattached Nova Scotian with access to care. So we launched VirtualCareNS.”
The organisation then went through a diligence process, looking at approximately 50 companies offering virtual platforms before selecting a provider. Today, patients can get same-day medical advice via their tablet, computer, or smartphone.
Integrated view for clinicians
“Nova Scotians were sent emails, encouraging them to participate and access care through VirtualCareNS. Once registered, they've been able to speak with a family doctor or nurse practitioner for health care advice, have prescriptions renewed, or get referrals as needed,” says Tomblin Murphy.
“We started in two areas of the province that had the highest number of people on the registry of patients without a provider. And then, because it was becoming very successful, very fast, we were asked to scale it quickly, province-wide.”
Enhanced use of analytics
The rapid onboarding of so many new patients to the virtual platform, however, would not have been possible without analytics to help understand and predict use rates.
“It's really important to understand when, how many, and what type of patient or person is going to need and use the service,” explains Murphy. “Only then can we develop a human resource strategy to meet the need efficiently and sustainably.”
Speeding up and adapting
But despite the rapid uptake and progress experienced, the journey is far from over. Murphy and his team see lurking issues, including the overall speed of the reporting service.
“The last few years, we've gone from three months to four hours for reporting. So there has been remarkable improvement, but with that, comes remarkable expectations and four hours was suddenly not quick enough,” he says.
“We knew where our databases were, but we didn't have the technical capacity to shrink that run time. We also knew what we would be able to do with real-time data. We simply didn't have the ability in-house to get there quickly enough; hiring new staff with the core competencies would take too long.”
Based on previous experience with EY Canada over the years, Nova Scotia Health knew they’d be able to sit down and sketch out a solution together. Murphy and his team worked alongside EY Canada’s technical teams to re-code the system and shrink run time from hours to minutes.
In addition, by working closely with EY Canada, Nova Scotia Health has been able to capitalise on data assets that were previously unavailable, including those around its human capital analytics.
“Within Canadian healthcare, as with other healthcare jurisdictions around the world, the compensation for our workforce accounts for anywhere from 60 to 80% of our budget and, within Nova Scotia, it's worth noting that the budget is over US$2bn,” says Murphy. “Until recently, we didn’t have access to a harmonised dataset covering both financial and human resources.”
Together, EY Canada and Nova Scotia Health have brought about the creation of this new data mart that would reconcile these existing systems.
Real-time insights
According to Maynard, real-time data insights are critical for any industry. They help identify ways to deliver better service, drive efficiencies, manage costs and deliver better and more timely care with improved safety, while presenting a more integrated patient journey map across care environments and practitioners.
But, based on EY’s global experience, real-time data is a challenge for many healthcare organisations, due to significant legacy systems that exist within them.
“The good news is there has been breakthrough capability through cloud computing and advanced technologies to be able to deliver integrated data without making a significant investment in re-platforming whole new systems.”
During the pandemic, Nova Scotia Health and EY Canada tackled the unprecedented problems that arose, from automation to workforce, resulting in new insights that allow them to understand not simply where they're spending money, but the driving reasons behind it.
“We learned significant lessons throughout the course of the pandemic,” says Murphy. “The last two years have been really difficult in healthcare with respect to the workforce. Understanding where we have potential gaps is essential to ensuring we have a sustainable system into the future.”
“The pandemic and the stresses it placed on healthcare organisations around the world created a massive capacity crunch, yet the business of healthcare had to go on. Robotics process automation was a really useful tool to help deliver the business of healthcare and maintain core operations while many of the staff had been redirected to emergency operations,” says Maynard.
During these challenging times, the EY team helped deliver intelligent automation solutions that leveraged machine learning and artificial intelligence capabilities to enable the system to quickly learn and adapt to the environment, acting as essential support for a key component of the business.
“That was a significant shift for us from an innovation perspective – to realise or address how we can keep providing services when the traditional mechanism of service delivery has been disrupted,” Murphy adds. “Again, the answer was wholesale digital transformation across the system.”
Thanks to its work with EY Canada, Nova Scotia Health has a clear vision of where it wants to be in the next five to 10 years.
“Historically, organisations have thought about private industry as funders,” says Tomblin Murphy. “We truly believe that private industries are partners, and so we engage them often. They're really important to the work that we are doing.”
To deliver on Nova Scotia Health’s longer-term vision, there will be significant investments throughout the transformation roadmap – from new clinical information systems to cloud computing capabilities, as well as new techniques to help produce insights and help clinicians and other organisational leaders utilise new innovations.
And, as the institution refocuses on how to provide better care for its residents, Murphy explains, it also aims to revamp the workplace to be more engaging and provide growth and opportunities for its employees and volunteers.
“It's not about using technology to eliminate positions. New technologies are faster and more efficient, often eliminating more tedious, manual processes and freeing up our workforce to do what they do best: practising the art and science of healthcare.”